Researchers worldwide are on a quest to stop the epidemic of dementia, a disorder of old age that leads to loss of cognitive abilites and full dependency on caregivers. Optimism followed the discovery of several risk factors for dementia that can be changed. Specifically, research from Western Europe and United States revealed that individuals with dementia are more likely those with shorter education, less stimulating jobs, higher rates of depression and cardiovascular risk factors. The purpose of the study was to investigate, which factors play a role for changes in cognitive health in the Czech Republic – a country previously underrepresented in this area of research.
Ongoing investigations suggests that changes in modifiable risk factors may be reducing cognitive decline and dementia. Specifically, several studies conducted mainly in Western Europe and the United States have suggested that age-adjusted prevalence and incidence of dementia has stabilized or declined during the past decade. These positive changes have been explained by increased levels of education, as well as better management of cardiovascular risk factors and diseases, such as high blood pressure, high blood cholester or diabetes mellitus. However, whether countries situated in Central and Eastern Europe achieved the same success, is unclear, as no country from this region contributed to the literature on this topic.
We aimed to fill in the knowledge gap about cognitive ageing in the Czech Republic – a country previously underrepresented in this area of research. We used two separate cohorts of individuals, derived from the 2006/2007 and 2015 wave of the Czech Survey of Health, Ageing and Retirement in Europe (SHARE) in order to compare 9 year changes in cognitive impairment. In our study, cognitive impairment was defined based on brief neurocognitive tests (verbal fluency, immediate recall, delayed recall, and temporal orientation) and may represent impairment of various severity – from milder impairment to dementia. Higher age is the strongest predictor of cognitive impairment. Therefore, it is essential to compare prevalences adjusted for age, which is what we have done in all comparisons. Overall, according to our most conservative estimate, we found that prevalence of cognitive impairment declined by one fifth, from 11% in 2006/2007 to 9% in 2015.
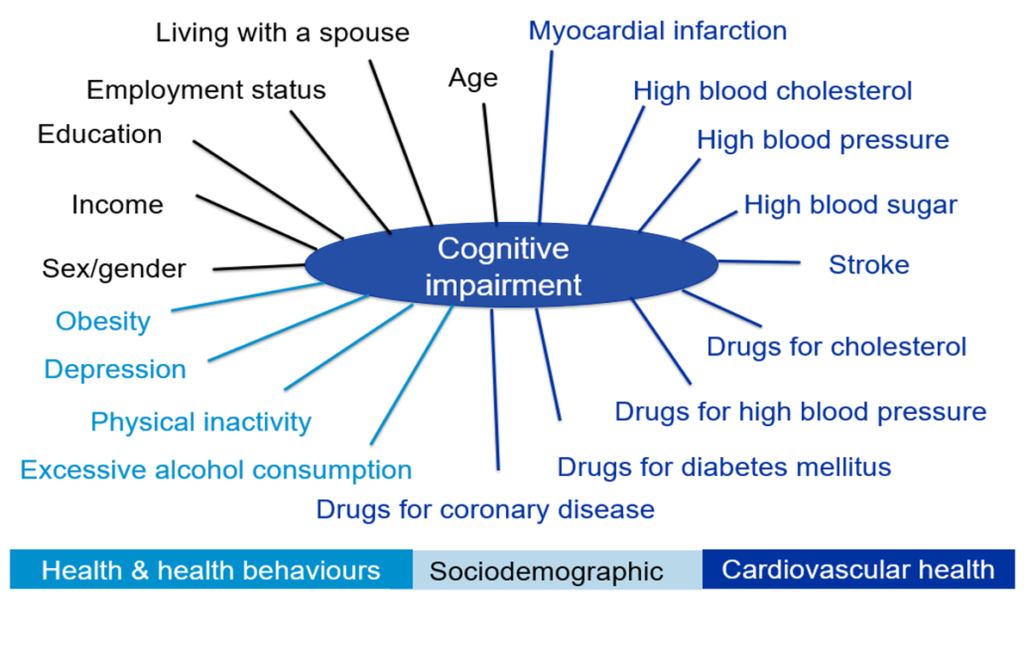
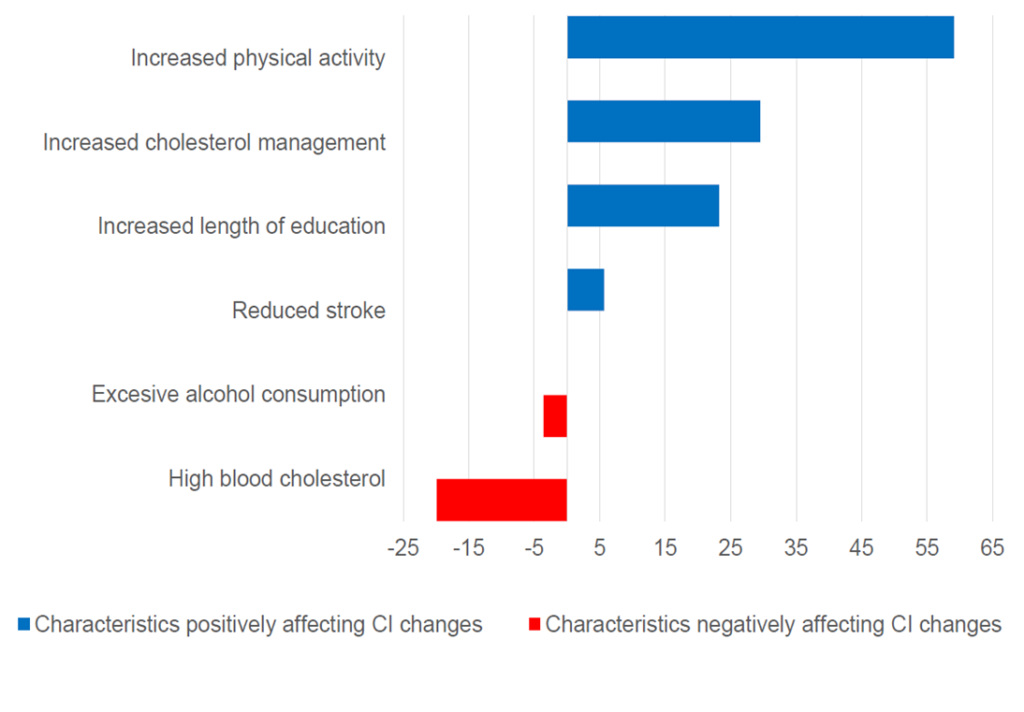
Our main interest was identifying which factors may have played a role for the observed changes, because countries in the Central and Eastern Europe have worse health profiles than countries in Western Europe. Further, after the end of communism, these countries have been undergoing rapid socioeconomic changes, which also likely influence health of the populations. We have examined many sociodemographic, health status and behaviours factors (Figure 1). Since we used two separate cohorts for our analysis, they have a different distribution of these characteristics. Thus, we could compare which ones explained the change by examining the differences in the profiles of the cohorts. We found that changes in distribution of six factors (Figure 2) were associated with the changes in cognitive health. The changes in age-adjusted prevalence of cognitive impairment could be explained through increased physical activity, length of education, cholesterol management, and reduced stroke. However, the 2015 cohort also had some characteristics that negatively influenced cognitive health. Specifically, they were more likely to have high blood cholesterol and alcohol consumption.
These findings have several important implications. Even though there is insufficient evidence from randomized controlled trials, a large body of observational studies – including our recent one – suggest that increasing length of education and reduction of cardiovascular risk factors and diseases could postpone the onset of cognitive impairment. This study brings indirect evidence that improvement can be achieved in a country situated in Central and Eastern Europe. Further work needs to be done to enhance positive health behaviours of the population. Namely, continuing improvements in physical activity, nutrition and cholesterol reduction could further contribute to additional improvement of cognitive functions of the population. To improve cognition of older adults, nationwide policies also need to aim at reducing alcohol consumption in the population.
About the authors:
First author: Dominika Seblova, Ph.D. – Columbia University, New York, USA
Last author: Pavla Cermakova, M.D., Ph.D. – National Institute of Mental Health, Klecany and Charles University Prague, Czech Republic
Other authors:
Prof. Carol Brayne, M.D., Ph.D. – University of Cambridge, United Kingdom
Vendula Machů, MSc. – University of Groningen, Netherlands
Bc. Marie Kuklová – National Institute of Mental Health, Klecany, Czech Republic
Miloslav Kopecek, M.D., Ph.D. – National Institute of Mental Health, Klecany, Czech Republic
The article is based on:
Seblova, Dominika et al. ‘Changes in Cognitive Impairment in the Czech Republic’. Journal of Alzheimer’s Disease, vol. 72, no. 3, pp. 693-701, 2019, DOI: 10.3233/JAD-190688











Leave A Comment