An update of the profile of older Europeans with dementia was performed with data from 18 countries. The findings of co-morbidity, high rates of drug intake daily and low levels of well-being irrespective of age should be considered in the assessment and management of dementia in the European population.
The increase in longevity due to the reduction of premature deaths has led to an increase of the number of people with dementia. There are different forms of dementia, the most common being Alzheimer’s disease. Although there are numerous studies about dementia and its related variables, some of the findings are contradictory. This generates doubt about some relationships and trends concerning the population with dementia (employment, health status, well-being and others) and how those relationships are linked with age progression compared to people without dementia. Furthermore, while research has documented developmental, lifestyle and cardiovascular risk factors associated with dementia, there is a dearth of research concerning the profile of individuals with dementia in terms of socio-demographic, behavioural and health variables. An assessment of these aspects might be relevant to consider for future dementia and research. The aim of this work was to analyze the profile of the European population with dementia aged 51 years or more using data from SHARE.
Participants were considered to have a diagnosis of dementia if they answered positively to the following question: “Doctor said you had: Alzheimer’s disease, dementia, senility” – Yes or No). Information on social-demographic, behavioural risks, health-related questions, cognitive function and mental health were collected.
A total of 45,340 European participants answered the question: “Doctor said you had: Alzheimer’s disease, dementia, senility” – Yes or No) of whom 2.0% (N=897) were identified has having a diagnostic of dementia. The proportion of participants with dementia varied from 0.7% in Switzerland to 4.4% in Spain. A slightly increased proportion was found among women. For participants under 75 years old the proportion of dementia cases was lower than 1%, increased about 3 times among those aged between 75 and 84 years old, and then again 3 times for those older than 84.
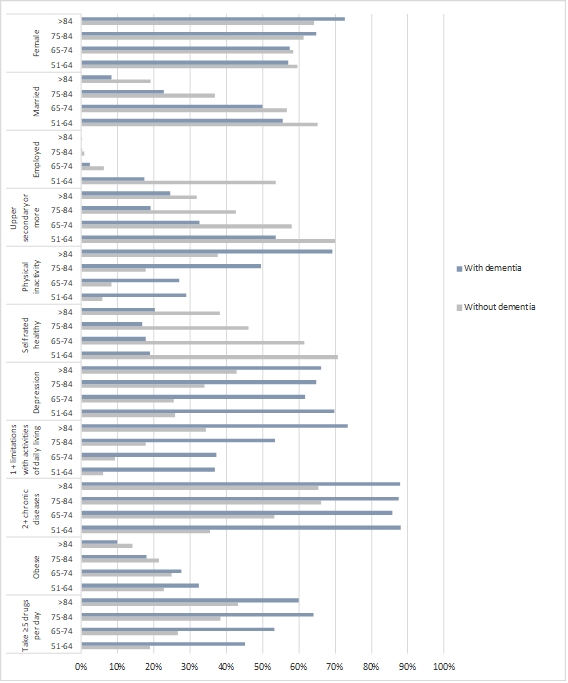
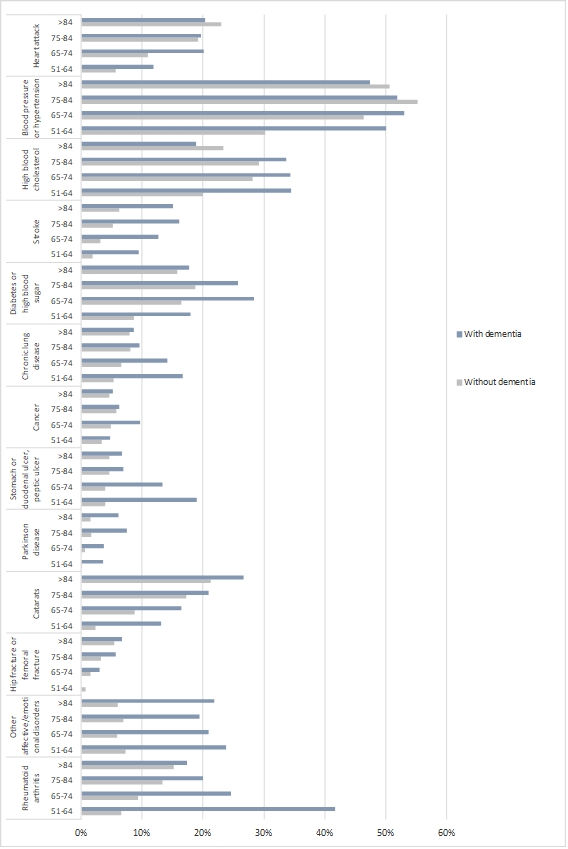
Socio-demographic characteristics across age groups for those having or having not been told by their doctor they had Alzheimer’s disease, dementia or senility can be found in Figure 1. Figure 2 shows the comparison of selected chronic diseases between Europeans with and without a diagnosis of dementia. In the group of participants with dementia the proportion of those with each one of the chronic diseases identified by SHARE was always higher than in the group without dementia, and the bigger differences were observed in the younger groups, those under 75 years old.
Our study contributes to the much needed research about dementia, given the burden and cost of this disorder. The planning of effective dementia interventions, must take into account that people with dementia have other comorbidities, and also other complex problems including cognition, neuropsychiatric symptoms, and activities of daily living. In our study, we performed an update to the profile of older Europeans with dementia based on the most recent available data of SHARE, a multidisciplinary and cross-national database that includes 18 European countries. In spite of having a diagnosis of dementia the majority of the participants were female, which follows the trend of life expectancy estimated in European countries, where women at age 65 have a longer life expectancy than men.
Age is considered to be the main risk factor in the development of dementia. When we analyzed dementia by age the results revealed that in those under the age of 75 the proportion of dementia cases was under 1%, increasing to 3.5% and 10.4% respectively in the age groups of 75 to 84 and over 84 years old.
This study shows that health and the well-being status of older Europeans with dementia are very unfavourable, regardless of their age. It was also verified that people with dementia: i) had a lower employment rate; ii) showed lower levels of formal education; iii) less were living a married life; iv) exhibited a moderate pattern of behavioural risks, but had higher levels of physical inactivity; v) had more chronic diseases and iv) higher intake of more than 5 drugs per day. The unfavourable health and well-being status of dementia subjects was found in all age groups. The high prevalence of co-morbidity, intake of more than five drugs daily, and low levels of well-being in the population with dementia requires the focus on interventions that consider people as a whole. Given the burden and cost of dementia, more research is necessary including the areas of prevention, treatment, cure and care. Medical, cognitive, emotional, psychological needs of people with dementia should be continuously assessed, so that care is improved with the course of dementia.
About the authors:

Maria Piedade Brandão, ESSUA – Health School, University of Aveiro, Aveiro, Portugal and CINTESIS – Center for Health Technology and Services Research, University of Porto, Porto, Portugal.

Margarida Fonseca Cardoso, ICBAS – Abel Salazar Institute of Biomedical Sciences and CIIMAR – Interdisciplinary Centre of Marine and Environmental Research, University of Porto, Porto, Portugal.
This article is based on:
Rafael Gonçalves Ferreira, Maria Piedade Brandão & Margarida Fonseca Cardoso (2018): An update of the profile of older adults with dementia in Europe: findings from SHARE, Aging & Mental Health, DOI: 10.1080/13607863.2018.1531385










Leave A Comment